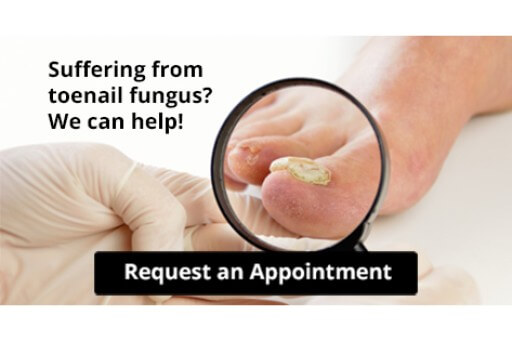
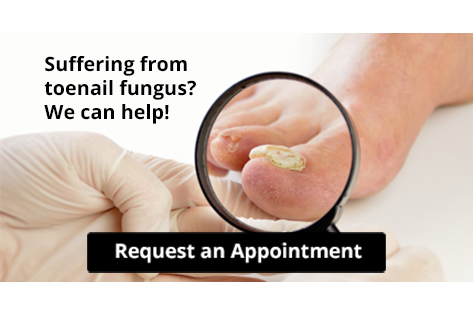
Choosing the right running shoe is vital for comfort and performance. There are four main types of running shoes, each designed to address different needs. Motion control shoes are ideal for runners who overpronate, offering extra support to prevent excessive inward rolling of the foot. Stability shoes provide moderate support and cushioning, making them suitable for runners who need a balance between comfort and stability. Neutral shoes are designed for runners with a neutral stride, providing cushioning without added support, perfect for those with a natural gait. Lastly, minimalist shoes aim to mimic barefoot running by offering minimal cushioning and support, encouraging a more natural foot movement. Understanding your running style and foot mechanics is key to selecting the right shoe, as it can help improve performance and prevent injuries during your runs. If you have sustained a foot or ankle injury while running, it is suggested that you consult a podiatrist who can treat various foot conditions, and guide you on what type of running shoe to purchase.
You should always make sure your running shoes fit properly in order to avoid injury. For more information, contact one of our podiatrists from Graff Foot, Ankle and Wound Care. Our doctors can provide the care you need to keep you pain-free and on your feet.
Choosing the Right Running Shoe for Your Foot Type
Improper shoe sizing can cause a myriad of problems for your feet. Shoes that don’t fit you properly can lead to muscular imbalances in your body, which can result in foot, knee, and hip injuries.
Tips for Finding the Right Running Shoe
- Make sure you have a thumb’s width of wiggle room between the end of your longest toe and the front of the shoe.
- There should be little to no slipping at the heel
- Don’t assume your size in one shoe brand will be your size in another
- Do not lace up your shoes too tightly
- Walk around in the store with your new shoes before you buy them
If you have any questions please feel free to contact our our offices located in Plano, Dallas, Prosper, Allen, Irving, Garland, Frisco, and Coppell, TX . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.